Glossectomy is the surgical removal of all or part of the tongue. The procedure is performed to treat cancer of the mouth, tongue and throat.
When a part of the tongue is removed, it is known as partial glossectomy whereas total glossectomy involves the removal of all of the tongue.
Anatomy of the Tongue
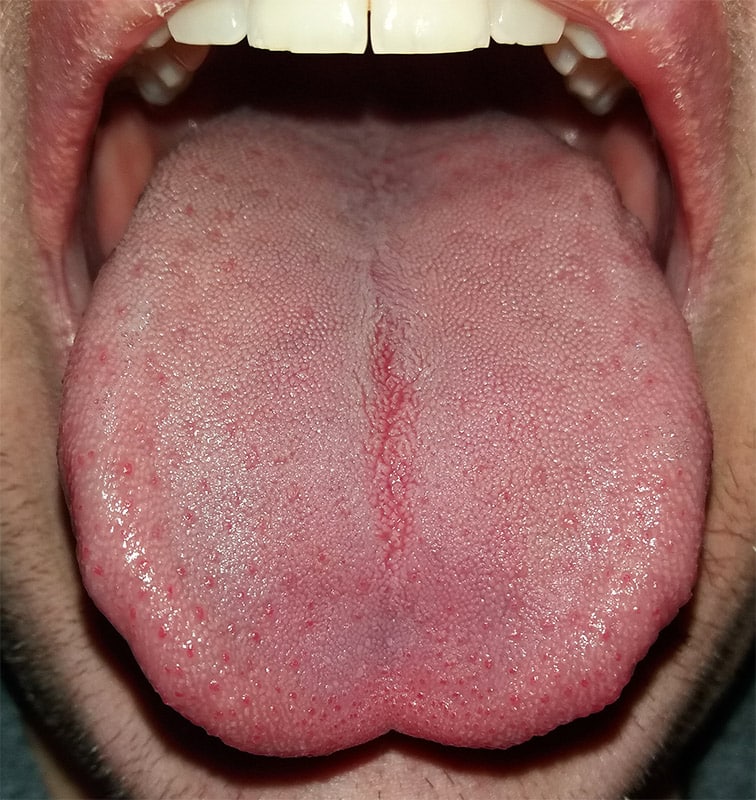
human tongue
The tongue is a muscular organ in the mouth that manipulates food for chewing and is used in the act of swallowing. The tongue also plays important role in speech. As a result of these critical functions, it is expected that there will be changes in swallowing and talking in patients who undergo glossectomy.
The human tongue is divided into two parts, an oral part at the front and a pharyngeal part at the back. The left and right sides are also separated along most of its length by a vertical section of fibrous tissue (the lingual septum) that results in a groove, the median sulcus, on the tongue’s surface.
Surgical Procedure for Glossectomy
In almost all cases, the patient will be put completely to sleep with general anesthesia. There may be a need for tracheotomy and/or a feeding tube, depending on the extent of the glossectomy and reconstruction.
There are a few different types of glossectomies, including:
Partial glossectomy: This is the removal of any part of the tongue, from a small part of the side or tip, an entire half of the tongue or even more.
Total glossectomy: This is the removal of the entire tongue, including the base of the tongue. This results in severe dysfunction with swallowing and resultant aspiration (food and liquids falling into the lungs).
A total glossectomy is performed along with a total laryngectomy in order to prevent aspiration and pneumonia. A total glossectomy will require major reconstructive surgery.
Associated procedures might include a tracheotomy, feeding tube placement, neck dissection, floor of mouth resection or mandibulectomy. A neck dissection is indicated for tongue/oral cavity cancers that go deeper than 3 or 4mm.
In addition, the extent of the reconstruction will depend on the amount of tongue and adjacent structures that are extracted.
Reconstructive options might be healing by secondary intention (letting it heal on its own), primary closure (placing stitches to close up the tongue that was removed), or flap reconstruction.
Related: What Is Esophagectomy All About?
The glossectomy can be done via a few different approaches depending on what part of the tongue needs to be removed, how much of the tongue needs to be removed and what associated procedures might be required.
i. Transoral – The surgical technique is used for small cancers and it can be performed entirely through the mouth
ii. Transoral robotic-assisted surgery (TORS) – For tumors at the base of the tongue, or oropharynx, a robotic-assisted surgical removal through the mouth might be an option.
iii. Transoral laser microsurgery (TLM) – In this technique, a laryngoscope placed through the mouth exposes various parts of the base of the tongue. A laser is then used to cut around the tumor to remove it.
iv. Mandibulotomy – For tumors in the base of the tongue or the back part of the oral tongue, your surgeon might recommend a mandibulotomy. This involves making a cut at or near the middle of the lower jawbone and swinging the jaw to the side to expose the back part of the tongue or the floor of the mouth.
v. Transcervical with pharyngotomy – This is another method to access the back part of the tongue and the base of the tongue. In this technique, an incision is made in the neck, and the neck is connected with the oropharynx through what is known as a lateral or medical pharyngotomy approach.
The tongue is pulled down into the neck, and the tumor from the back part of the tongue can be removed without having to cut the jawbone.
Risk and Complications
Like every surgical procedure, there is a risk of complications with glossectomy. Some of the possible complications include:
Bleeding, including hematoma: If there is severe bleeding after the procedure, your surgeon might need to quickly take you back to the operating room to stop the bleeding.
Infection: The tongue has a wonderful blood supply and infections of the tongue are extremely uncommon. Still, as with any surgical procedure, there is always the risk of an infection after the surgery, particularly if the glossectomy is associated with additional procedures that might connect the mouth with the neck. This might require antibiotics and/or drainage of the infection.
Dysarthria, or difficulty speaking: The extent to which your speech is affected will depend on how much and what part of the tongue is removed. You might work with a speech and swallowing therapist to improve your function.
Dysphagia, or difficulty swallowing: The extent your swallowing is affected will depend on how much and what part of the tongue is removed. You might work with a speech and swallowing therapist to improve your function.
Aspiration: After the removal of a large part of your tongue, particularly the base of the tongue, it might be difficult to control your swallow mechanism. This can lead to saliva, drinks and food falling into your voice box and into your lungs, which can lead to pneumonia. You should work with a speech and swallowing therapist to improve your function.
Salivary fistula: This term is used to describe when saliva is leaking from the mouth into the neck. The chances of this increase if you have had previous treatment, including radiation and/or chemotherapy because healing of wounds might be impaired in these cases.
Typical treatment for this is to place a drain to divert the saliva away from critical structures in the neck and later to place packing into that diverted track to let the body heal it up on its own. In some cases, an additional surgical procedure might be required to close the leak.
Recovery
This surgery takes about two hours to complete and requires a week’s stay in the hospital. Recovery can take several weeks, during which your doctor may recommend restricting activities.
Glossectomy Outcomes
Studies have shown that patients with cancer of the oral tongue who are under surgical resection and reconstruction experience impairments in function and quality of life.
However, in the long term declines in swallowing function and most qualities of life domains related to the head and neck returned to normal levels by 1-year post-operation, while difficulties with dry mouth and sticky saliva persisted.
Read More: Scalenectomy