Bankart Repair – Overview
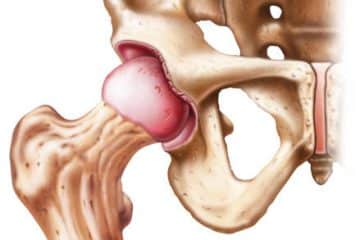
A Bankart lesion is a tear in the anterior portion of the shoulder’s glenoid labrum. Repetitive anterior shoulder subluxations cause this condition.
The connective tissue circle around the glenoid labrum can be damaged by anterior shoulder dislocation. It can also cause damage to the labrum and capsule connection.
It’s usually due to a lack of or improperly constructed medial glenohumeral ligament. Volleyball, tennis, and handball players, and those who engage in overhead exercises are all susceptible to this injury.
To restore safety and stability to the shoulder, a Bankart repair entails re-anchoring and suturing the damaged portion of cartilage.
This operation is usually done arthroscopically in an outpatient surgery clinic, which means patients go home a few hours after the procedure is finished.
Preoperatively, patients describe pain or occasions where the ball may fall out of the joint in certain positions or during particular actions If the injury is not treated, the slippage may continue and become more common.
When an anterior labrum injury occurs, a Bankart repair is one of the minimally invasive, tissue-sparing alternatives we use to manage shoulder instability.
This is one of the most effective strategies to improve the shoulder’s stability and comfort.
The procedure’s purpose is to reconnect and straighten the shoulder’s damaged labrum and ligaments. The surgeon does this by inserting an arthroscope into a small incision.
Types of Bankart Repair
1. Soft Tissue Bankart Repair Procedure
The procedure is almost always done arthroscopically when there is no glenoid fracture or only a little one along with the labral tear. This enables for better imaging of the damage and less disruption of tissues that aren’t involved.
Suture anchors are utilized to secure the labrum to the glenoid. These are very little devices that are placed into the glenoid at the attachment point.
Tiny strands are incorporated into these anchors. The labrum can be attached to the desired spot. A little bone fragment can be included in the repair if it is present.
2. Bony Bankart Repair Procedure
A bony Bankart lesion occurs when a bigger fracture to the bottom, front of the glenoid is linked with the labral tear.
Many of these injuries can still be treated arthroscopically, with suture anchors used in the same or somewhat different ways.
However, the bone fragment might be quite large in some cases. This may necessitate the use of a pin or two to repair the fracture. This can sometimes be done using laparoscopic surgery, but maybe an open incision is required.
Bankart Repair Procedure
1. Preoperative Preparation
The first step in evaluating a patient with shoulder instability is to take a complete medical history. It’s critical to learn about the injury source, the direction of the instability, and the method of treatment.
2. Posture and Anesthesia
This comprises preoperative nerve block and insertion of a continuous catheter for postoperative pain management.
The patient usually placed in the lateral decubitus position
3. Placement of Portals and Diagnostic Arthroscopy
To enter the shoulder joint, an incision is made and an arthroscopic needle is used. Using spinal needle localization, two anterior working portals are then established in the rotator interval from the outside in.
4. Preparation of Glenoid
The labrum is elevated and freed up from the anterior glenoid, which is commonly scarred down in a nonanatomic, medialized position, using a 30◦ c arthroscopic tissue liberator.
Since insufficient mobilization of the anterior labrum from the glenoid neck can result in a nonanatomic, less functional restoration, this is a crucial phase.
5. Capsulolabral Plication and Anchor Positioning
The drill guide for the suture anchor is inserted through the inferior cannula and positioned on the face of the glenoid as near to the 6 o’clock position as feasible while seeing from the posterior portal.
6. Sequential Anchor Placement and Knot Tying
To avoid articular cartilage injury from the suture, knots are tied arthroscopically using low-profile sliding locking Westin knots followed by half hitches with care to keep the knots away from the glenoid face.
Depending on the patient’s size, a minimum of 4 to 6 anchors are employed. The anchors are set as close together as possible without endangering the prior anchor’s fixation.
7. Closure of the skin and immobilization of the shoulder
To close the skin, nonabsorbable sutures are utilized. Surgical incisions are dressed with sterile cloths. Patients are moved to the recovery area while wearing a shoulder immobilizer.
Complications
- Recurrence of the instability
- Hemorrhage
- Infections
- Thrombosis
- Tightness in the shoulders
- Trauma to a blood vessel or a nerves
Post-operative Recovery
Sutures and other fixation devices are simply utilized to keep the restored tissues in place. These reconstructed structures must still heal in place. If not, the fixation will eventually fail, and the tissues will revert to their pre-surgery state.
Excessive shoulder mobility and abrupt injuries can increase the likelihood of failure. As a result, a sling is frequently required for the first 4-6 weeks following surgery.
Physical treatment is needed by the majority of people. Postoperatively, many of my patients spend 5 to 6 months in physical therapy. Initially, the therapy aids in the reduction of discomfort and edema. Later on, it can help you regain your range of motion, power, and functionality.
Power and range of motion must be sufficient before contact or dangerous activities are allowed.
This usually takes at least six months. Full healing, on the other hand, can span anywhere from 7 months to a year.
References
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5495990/
https://orthop.washington.edu/patient-care/articles/shoulder/bankart-repair-for-unstable-dislocating-shoulders.html
https://www.arlingtonortho.com/conditions/shoulder/shoulder-arthroscopic-bankart-repair/
See Also

Dr.Sharif Samir Alijla, is a general medical doctor and a well-rounded professional that cares and treats patients from Palestine. I participated in many medical studies and conferences, I've launched a range of community initiatives and taken part in a variety of leadership and change training programs. I worked as an author for many medical websites such as TebFact . I specialized in writing medical articles from authoritative and updated sources in a simple and smooth the way for the reader.