Emergency hernia surgery
Abdominal wall hernias are one of the most common conditions encountered by surgeons. More than 2.3 million abdominal hernia repairs took place in U.S hospitals alone in the first decade of the 21st century.
Approximately 25% of these procedures were performed emergently. Why do hernias develop? What are the types of hernia? When it becomes an emergency? And how can we treat them? In the article below you will find answers to these questions and more.
What is hernia?
The abdominal wall, consisting of muscles and aponeuroses, has a number of functions, one of which is to keep the internal organs in a natural position and resist the intra-abdominal pressure they create.
A hernia is a disease in which the organs of the abdomen extend beyond the cavity through the weak points of the abdominal wall. Activities and medical conditions that increase pressure on the abdominal wall can lead to a hernia.
Here are some factors that contribute to this process:
- Excessive physical exertion (such as heavy weight lifting)
- Severe chronic cough (smoker’s cough)
- Straining (due to long-term constipation)
- Diseases in which people experience shortness of breath with difficulty of breathing out (bronchial asthma)
- Excess body weight Almost any organ of the abdominal cavity can herniate – intestinal loops, bladder, an omentum, less often the stomach, extremely rarely even the liver and spleen.
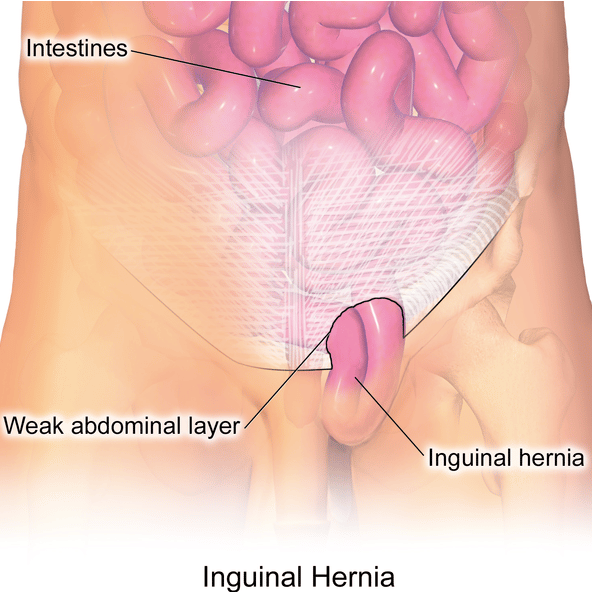
Emergency Hernia Surgery
Types of hernia
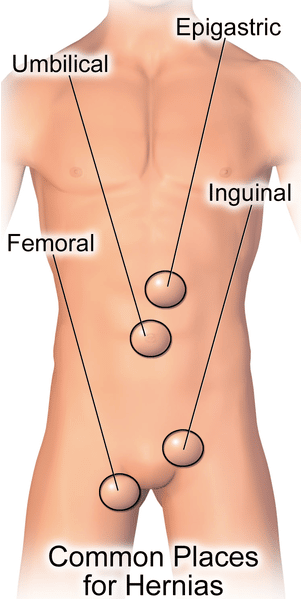
Emergency Hernia Surgery
Hernias are mostly found in the groin, navel and upper stomach areas. They are further classified according to their precise anatomical location and nature. Amongst the most common types are :
Inguinal hernia – bulge on the pubic bone. Most widespread type, more than 70% of hernias are inguinal.
Femoral hernia – bulge in the groin area or upper thigh
Umbilical hernia – happens when intestines protrude through weak abdominal muscles near the belly button
Hiatal hernia – in this type of hernia part of the stomach elevates into thorax through the defect of diaphragm. This is an example of internal hernia, protrusion remains within the abdominal cavity, as opposed to other hernias in this list.
Incisional hernia – any previous abdominal surgery can lead to incisional hernia through the scar.
When it becomes an emergency
Another way to classify hernias is their nature, or in other words, whether or not patients are able to reduce the mass back into the abdomen.
Reducible hernias can be pushed back into the opening. Small reducible hernias may not cause any symptoms at all.
It might take years before they begin to cause noticeable symptoms like pain and discomfort. The only treatment is surgery.
Large mass, long-term pain, discomfort during exertion, enlargement of hernia, irritation and numbness due to nerve compression – these findings indicate the need for elective surgery. But in some cases reducible hernias may never cause so many negative symptoms to warrant surgery.
Irreducible (incarcerated) hernias can not be pushed back into the abdominal cavity. This indicates that herniated tissue got trapped.
Usually incarceration of hernia causes a fair amount of pain, but sometimes pain can be mild and patients may be lulled into a sense that it is not urgent. But it should always be treated as soon as possible as it can easily strangulate.
After incarceration, the next step might be a strangulated hernia, when the blood supply to herniated tissue gets cut. It is a complication, rather than a hernia type. This is an emergency of the highest order. Emergency hernia repair is needed.
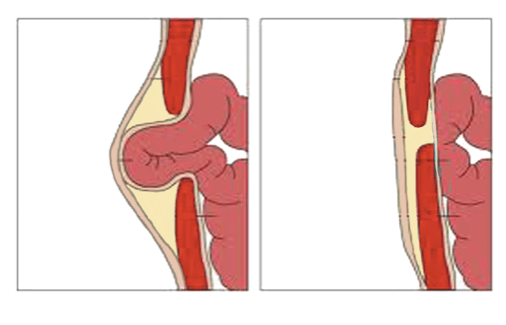
Emergency Hernia Surgery
Surgery
More than 300 methods of hernia repair are known. Different types of hernia require different surgical approaches, but all of them can be divided into two groups: Herniorrhaphy and Hernioplasty.
Herniorrhaphy (tissue repair)
Developed in the second half of the 19th century and still widely practiced, it is the oldest type of hernia surgery.
Surgeon makes a long incision over the hernia, cuts tissues and gains access to hernial sac. Then the displaced organ is returned to its original position and hernial sac is removed. After that the surgeon stitches the sides of the hole together.
The distinguishing feature of this approach is the closure of the herniated orifice by the patient’s own tissues (muscles, fascia and aponeuroses).
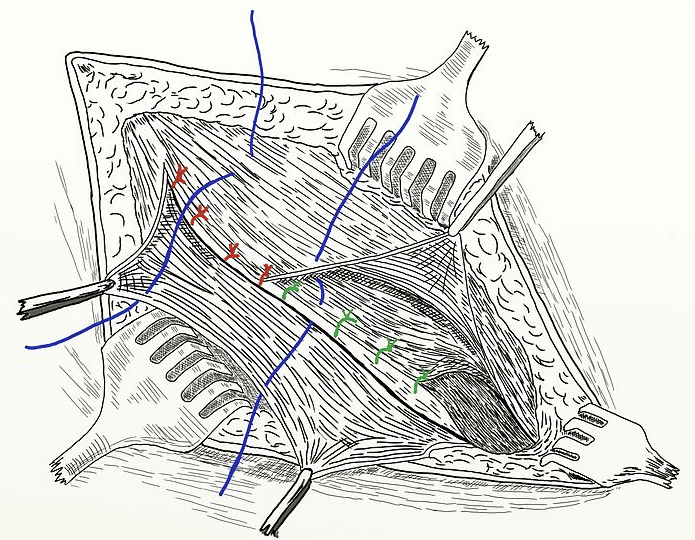
Emergency Hernia Surgery
Recovery and recurrence – The frequency of recurrence of hernias after these operations varies from 20% to 70%, depending on the condition of the patient’s tissues and the correctness of surgeons choice.
The main disadvantages are postoperative pain on the first days after surgery due to tissue tension and long periods of physical rehabilitation. Intense physical activity is contraindicated for at least 3 months after surgery.
Hernioplasty (mesh repair/tension free-repair)
In this method, instead of instantly stitching the muscle opening, the surgeon first covers it with a mesh made of synthetic plastic.
Small cuts are made around the hernia opening and the mesh is stitched into the healthy surrounding tissue. Weak and damaged tissue around the hernia can then use this mesh as a support to regrow and gain strength.
Methods of plastic surgery “without tension” of the patient’s own tissues have existed since the second half of the 1960s. But these methods have gained great popularity in recent years, mostly due to the creation of perfect synthetic materials and the development of new techniques for closing the hernial orifice.
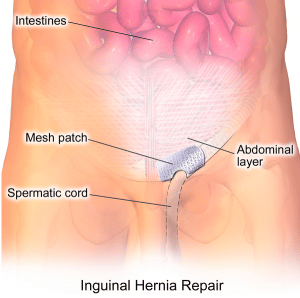
Emergency Hernia Surgery
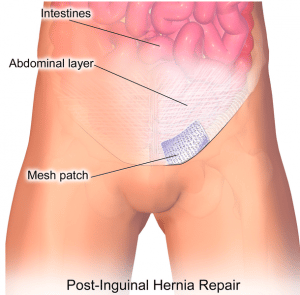
Emergency Hernia Surgery
Recovery and recurrence – The recurrence rate does not exceed 1% in specialized clinics, regardless of the type of hernia. The pain syndrome after surgery is minimal, as there is no tension on patients’ own tissues.
Intense physical activity is possible a month after the operation, household physical activity is not limited. This allows healthcare providers to perform such operations on an outpatient basis.
Another positive aspect is the possibility of performing the operation under local or spinal anesthesia, which is especially important for elderly patients and patients with heart and lung diseases.
Emergency Hernia Surgery
Due to its reliability and simplicity, this approach is most widespread for hernioplasty with inguinal hernias. It is applicable for any type and size of inguinal hernias.
Laparoscopic (keyhole) surgery
Not all approaches require a direct cut above the hernia. During laparoscopic surgeries doctors make small keyhole incisions and use a tiny video-camera device that allows direct visualisation of intra abdominal space.
In most cases, the abdominal wall defect is closed from the inside of the abdominal cavity with a synthetic mesh prosthesis. Since it is a minimally invasive procedure, tissues take less damage.
Another advantage is the possibility of performing bilateral plastic surgery and combined operations in the abdominal cavity through the same punctures, if needed.
On the other hand, disadvantages of the methods of this group include general anesthesia and the need to inject gas into the abdominal cavity to create an operative space (dangerous in patients with diseases of the lungs and heart).
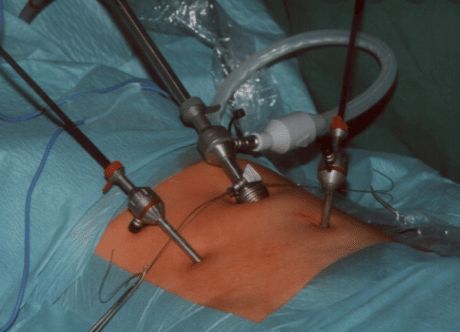
Emergency Hernia Surgery
Recovery and recurrence – The frequency of hernia recurrence after this repair is 2-5% and is determined by the type of hernia and the skills of the surgeon.
Important advantages of these methods are low trauma, which means insignificant pain syndrome after surgery. It also requires short rehabilitation periods, up to a month.
Take-home points
While most hernias can be managed with elective surgeries, some may require urgent intervention. If your hernia can not be pushed back to the abdominal cavity it may be incarcerated and you should see a doctor immediately, as it tends to strangulate.
Symptoms of a strangulated hernia include sudden worsening of pain, fever, vomiting, nausea or discoloration of hernia bulge.
There is no time to wait for a doctor appointment here, you should seek emergency medical care. Luckily, hernia surgeries are fairly safe and effective procedures.
See Also
References:
https://jamanetwork.com/journals/jamasurgery/fullarticle/2089144
https://next.amboss.com/us/article/030eSf?q=hernias
https://www.msdmanuals.com/professional/gastrointestinal-disorders/acute-abdomen-and-surgical-gastroenterology/acute-abdominal-pain
https://wjes.biomedcentral.com/articles/10.1186/s13017-017-0149-y
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1963533/