Mastectomy refers to the surgical removal of one or both breasts, partially or completely. A mastectomy is usually carried out to treat breast cancer. People at high risk of developing breast cancer may undergo the procedure as a preventive measure. Similar breast surgery is the lumpectomy. Lumpectomy is the surgical removal of a breast lump instead of the whole breast. Choosing between mastectomy and lumpectomy can be difficult. Both procedures are referred to as “local therapies” as they target the area affected by cancer as opposed to “generalized therapies” like chemotherapy and hormone therapy. They are both effective in the treatment of breast cancer. However, not everyone can undergo a lumpectomy in lieu of mastectomy due to a range of factors.
Medical Uses of Mastectomy
Mastectomy is the preferred method of treatment of breast cancer in a certain group of patients as in:
– Previous Radiation Therapy: People who have already had radiation therapy to the affected breast may be more suitable for mastectomy.
– Affected Areas: People with two or more distant areas of cancer in the same breast are more suitable for mastectomy. Also, the size of the tumor is a factor to consider as tumors larger than 5 cm have poor prognoses for a lumpectomy.
– Diseases: Some people have certain connective tissue diseases which make them highly sensitive to side effects of radiation therapy, e.g. scleroderma, lupus, etc. People with such diseases are more suitable for mastectomy.
– Pregnancy: Radiation may have serious adverse effects on the unborn child. Hence, pregnant women are better served by traditional mastectomy procedures.
Types of Mastectomy
Now, there are several surgical approaches to mastectomy. The type that a person decides to undergo depends on factors such as the size, location, and behavior of the tumor, etc.
There are five different types of mastectomy namely; Simple or total mastectomy, modified radical mastectomy, radical mastectomy, skin-sparing mastectomy, nipple-sparing (subcutaneous) mastectomy.
Simple Mastectomy (total mastectomy) – In this procedure, the surgeon concentrates on the breast tissue itself and the entire breasts tissue is removed. The lymph nodes of the axillary area (armpit) are not removed. The procedure is simple compared to the other types of mastectomy and is appropriate for people who women seeking prevention of breast cancer. People who undergo a simple mastectomy can usually leave the hospital after a brief stay.
Radical mastectomy – This procedure is also known as Halsted mastectomy and was first performed in 1882. It involves the removal of the entire breast, the axillary lymph nodes, and the pectoralis major and minor muscles behind the breast. This procedure provides no survival rate for most tumors. The procedure is reserved for tumors involving the pectoralis major muscle and recurrent breast cancer affecting the chest wall. Radical mastectomy is reserved for such cases as the procedure can be disfiguring as much as the tumors.
Modified radical mastectomy – This involves the removal of entire breast tissue along with the axillary lymph nodes and the pectoral muscles are undisturbed.
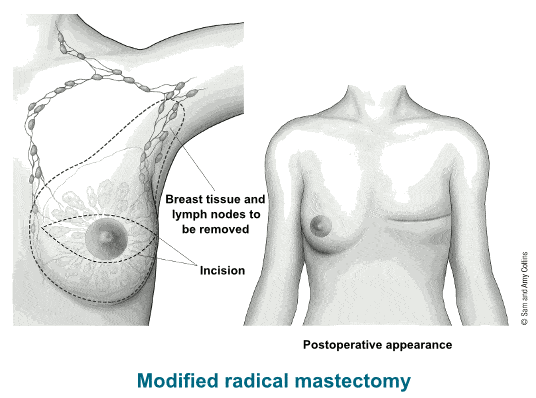
This type of mastectomy is used to examine the lymph nodes because this helps to identify whether the cancer cells have spread beyond the breasts
Skin-sparing mastectomy – In this surgery, the breast tissue is removed through a conservative incision made around the areola (the dark part surrounding the nipple). The increased amount of skin preserved as compared to traditional mastectomy resections serves to facilitate breast reconstruction procedures. People with cancers that involve the skin, such as inflammatory cancer, are not suitable for skin-sparing mastectomy.
Nipple-sparing (subcutaneous mastectomy) – Breast tissue is removed, but the nipple-areola complex is preserved. Candidates suitable for nipple-sparing mastectomy are women whose tumor does not involve the nipple or tissue under the areola and whose tumors are surrounded by a clear margin of cancer-free tissue.
Before Mastectomy Surgery
Before the operation, everyone will meet with the surgeon for a few days.
The patient is given enough time to reflect following after the initial shock of hearing the cancer verdict. Most importantly, the patient will decide whether the entire breast is to be removed or only a part of it.
The perspective of not having the breast is very painful and difficult to accept. The support of the family and friends of the patient is crucial at the point to enable the patient to make a good decision.
The surgeon will stress the statistical fact of much better chances of cure and survival when the breast is removed completely.
Before the surgery the person will have time to ask any questions regarding the procedure at this time and after everything is addressed a consent form is signed. Information about not eating or drinking anything beforehand will be gone over as well. The person will also meet with the anesthesiologist or the health professional who is going to be giving the anesthesia the day of the operation.
During Mastectomy Surgery
Mastectomy is an extensive procedure and it is usually performed under general anesthesia. This implies that the patient will be asleep while the operation is going on. The patient will be hooked up to an ECG machine to monitor vitals and the heart rhythm throughout the whole surgery.
After Mastectomy Surgery
When the procedure is complete the patient will be taken to a recovery room where they are monitored until they wake up and their vital signs remain stable. It is normal for people that have mastectomies to remain in the hospitals for 1 to 2 nights and they are released to go home if they are doing well. The decision for discharge should be made by the doctor based on the person’s overall health at the time. The person is dressed with a bandage over the surgery site that is wrapped around the chest snugly.
It is common to have drains coming from the incision site to help remove blood and lymph to initiate the healing process. Patients may have to be taught to empty, care for, and measure the fluid from the drains. Measuring the fluids will help identify any problems the doctors need to be aware of. Patients should be taught the effects of the surgery, such as regular activity may be altered.
There is a possibility that pain, numbness, or tingling in the chest and arm could continue long after the surgery has been done. It is recommended that patients see their surgeon 7–14 days after the surgery, during this time the doctor will explain the results and talk about further treatment if needed such as radiation and chemotherapy.
The doctor might refer the patient to a plastic surgeon if she showed interest in breast reconstruction surgery.
Side Effects of Mastectomy
Following a mastectomy procedure, some risks and side effects may include:
– Change in shape of the breasts: This may cause painful psychological effects on the patient.
– Infection: The surgical site may become infected with bacteria, fungi, or other microorganisms.
– Hematoma – This is the build of blood in the wound
– Seroma: This is the buildup of clear fluid in the wound
– Bleeding
Contact your doctor immediately at the first sign of infection, including redness, tenderness or unusual swelling at the surgical site, or fever.